
While there are many public health issues, there are also scores of victories. Primary prevention of tooth decay, through the fluoridation of water, is one of public health’s biggest success stories.
Mystery Ingredient in the Water

"The Colorado Brown stain" perplexed dentists in the 1900s when they saw that Colorado Springs natives all appeared to have chocolate-stained teeth. Yet, as dentists Dr. Frederick McKay and Dr. G.V. Black discovered, the browning of the teeth, or mottled enamel, provided protection from common tooth decay.
Dr. McKay was asked to investigate a town in Idaho where parents were growing concerned about their children suddenly exhibiting brown stains. He hypothesized that there must be something in the water as the town had recently changed their water supply to a nearby warm springs. Upon following his suggestion to revert to the old water source, the children’s permanent teeth were no longer brown.
Dr. Churchill, a chemist, tested the local waters of Bauxite, PA, after Dr. McKay published his findings from Idaho, Colorado and Pennsylvania. Churchill was flabbergasted when he was first alerted about his own findings, prompting him to believe his assistant had contaminated the sample. He exclaimed, “Whoever heard of fluorides in the water?”
The Role of Fluoride
Because naturally occurring fluoride minerals can be found in freshwater and saltwater, the scientists found themselves confronted with the Goldilocks principle: too much fluoride and the children ended up with fluorosis (brown teeth), but too little, and the children suffered tooth decay. The findings launched an investigation by the National Institutes of Health (NIH) that sought to understand the optimal level of fluoride that would protect teeth from caries without causing mottled enamel.
In 1962, Francis Arnold Jr. published a study looking at 15 years of fluoridation from Grand Rapids, Michigan, the first city to officially fluoridate its water. The study carried validity with its large sample size of over 25,000 children. The findings were that the incorporation of fluoride was correlated with a 57 percent reduction of caries rate among the children born after its addition.5 The Grand Rapids findings led many dentists, the Centers for Disease Control and Prevention, and the NIH to more definitively believe that fluoride prevents dental caries. This scientific breakthrough revolutionized oral health, making the chronic disease, dental caries, preventable.
Prevention or Treatment?
According to Dr. Greg Olson, an expert dentist here at Loma Linda, fluoride that is ingested becomes part of the tooth structure and helps build the tooth, thus acting as the primary agent against tooth decay. Topical fluoride, on the other hand, can help with the process but at a much smaller scale. Thus, we need a combination of both systemic and topical. He stressed the importance of dental care for a large number of those who were already suffering from oral health problems.6
Yet, as of 2014, only 74.4 percent of Americans have access to fluoridated water through public water systems.7 Many states are below average, with only 64 percent of California receiving fluoridated water through community water systems in 2012.7
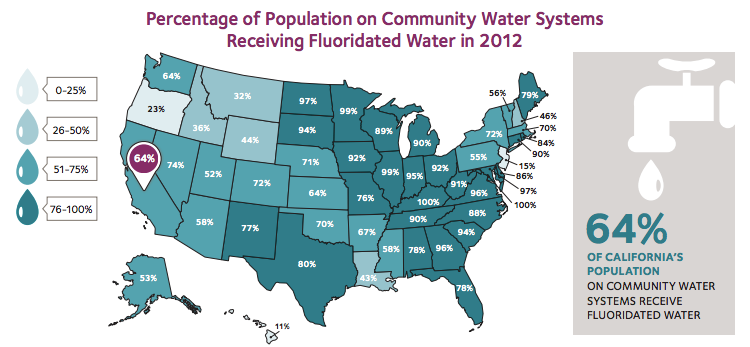
Figure 1. Percentage of Population on Community Water Systems Receiving Fluoridated Water in 2012 (American Dental Association)8
At first, I thought that much of this was due to lack of funding. I later discovered that the story was much more complicated and rang an all-too-familiar bell.
The Anti-Fluoridation Movement
Just as public health initiatives have faced strong opposition from the likes of anti-vacciners, it now also faces an anti-fluoridation movement. The Fluoride Action Network is a project run by doctors, lawyers, and dentists who all believe that we are given toxic levels of fluoride that could harm our health. The website tracks numerous communities that have chosen to have fluoride removed from their water source. It also cites over 50 studies that observe the relationship between fluoride and IQ.
However, many of these research papers have flaws that threaten their internal validity. Some of these papers have small sample sizes while others fail to look for additional factors that could affect the outcomes. For instance, data may show that over the past 50 years, more cities have put fluoride in their water or that cities went from no fluoride to the recommended levels of fluoride. Then, they look to see if the prevalence of autism has increased over the past 50 years. Lo and behold, it has. You cannot, however, attribute the rise in autism to the increase in fluoride based on such a study design. Correlation does not equal causation. Additionally, prevalence of autism may have artificially gone up because of improved diagnostics. Researchers at Columbia University and the Institute for Evaluation of Labour Market and Education Policy (IFAU) in Sweden did not find evidence of relationships between fluoride and IQ.9
There is something to be said, however, about the amount of fluoride we ingest and fluorosis, a chronic condition that can be caused by excessive intake of fluoride. Since the 1960s, the standard for water fluoridation levels was set to 0.7 parts per million for warm climates and 1.2 parts per million for cooler climates. In 2011, the Environmental Protection Agency (EPA) and the Department of Health and Human Services (DHHS) released a statement that they were going to reassess their recommendation.10 This announcement came two months after the CDC published its findings that there was a 40.6% prevalence of fluorosis amongst 12-15 year olds. The overall prevalence for people between the ages of 6-49 was less than 25%.11 In 2015, DHHS issued the final recommendation that the level of fluoride should be 0.7 ppm throughout the country. The decision was based on the fact that the fluorosis incidence and prevalence was mostly a mild form that actually led to white marks in the teeth, possibly because people receive fluoride from multiple sources such as diet.12,13 Since the initial announcement, over 50 communities in the United States stopped fluoridating their water and continue to do so.14 Many European countries have also decided against water fluoridation for a variety of reasons and some provide alternative sources such as fluoridated salt.15
I can empathize with the fear that such news can spark, but I urge citizens to understand that discontinuing fluoridation altogether can exacerbate the racial and socioeconomic oral health disparities that are already present despite the decreasing rates of dental caries. 16,17
While there remains much debate over whether or not to fluoridate our water, one thing that should not be up for debate is the importance of access to dental care. It is encouraging to know that California’s Senate Bill 562: The Healthy California Act, does include dental insurance for all.18
Author Bio:

Priya Vedula is a health policy analyst at the Institute for Health Policy and Leadership. Her work involves examining health policies and regulations with a focus on oral health, mental/behavioral health, and hunger. She received her Master of Public Health degree from Columbia University.
References:
- https://www.epa.gov/sdwa
- https://www.npr.org/sections/thetwo-way/2016/04/20/465545378/lead-laced-water-in-flint-a-step-by-step-look-at-the-makings-of-a-crisis
- http://www.wnem.com/story/30995770/united-way-estimates-cost-of-helping…
- Mona Hanna-Attisha, Jenny LaChance, Richard Casey Sadler, Allison Champney Schnepp, “Elevated Blood Lead Levels in Children Associated With the Flint Drinking Water Crisis: A Spatial Analysis of Risk and Public Health Response”, American Journal of Public Health 106, no. 2 (February 1, 2016): pp. 283-290.
- Arnold FA Jr, Likins RC, Russell AL, Scott DB: Fifteenth year of the Grand Rapids fluoridation study. J Am Dent Assoc 1962;65:780–785.
- Newbrun, E. (2004), Systemic Benefits of Fluoride and Fluoridation. Journal of Public Health Dentistry, 64: 35–39. doi:10.1111/j.1752-7325.2004.tb02775.x
- https://www.cdc.gov/fluoridation/statistics/2014stats.htm
- https://www.ada.org/~/media/ADA/Science%20and%20Research/HPI/OralHealthCare-StateFacts/California-Oral-Health-Care-System.pdf
- https://www.ifau.se/globalassets/pdf/se/2017/wp2017-20-the-effects-of-fluoride-in-the-drinking-water.pdf
- https://wayback.archive-it.org/3926/20140108162323/http://www.hhs.gov/news/press/2011pres/01/20110107a.html
- https://www.cdc.gov/nchs/data/databriefs/db53.htm
- http://www.ada.org/~/media/EBD/Files/PHS_2015_Fluoride_Guidelines.pdf?la=en
- https://www.ars.usda.gov/ARSUserFiles/80400525/Data/Fluoride/F02.pdf
- http://fluoridealert.org/content/communities_2010/
- Árnadóttir, I. B., Ketley, C. E., Van Loveren, C., Seppä, L., Cochran, J. A., Polido, M., Athanossouli, T., Holbrook, W. P. and O'Mullane, D. M. (2004), A European perspective on fluoride use in seven countries. Community Dentistry and Oral Epidemiology, 32: 69–73. doi:10.1111/j.1600-0528.2004.00142.x
- https://www.nidcr.nih.gov/DataStatistics/SurgeonGeneral/Report/NewsRelease05252000.htm
- https://www.nidcr.nih.gov/DataStatistics/FindDataByTopic/DentalCaries/D…
